During spontaneous perimenopause, estrogen (really estradiol or E2) levels fluctuate wildly before they decline completely when a woman enters into menopause or postmenopause. If a woman doesn’t have this steady decline and instead has her ovaries surgical removed, experiencing primary ovarian insufficiency, or has damage to her ovaries from medications or radiation, she enters this estrogen deprived state rather swiftly. Either way, the effects are still similar in the brain, and this is known as The Estrogen Withdrawal Theory. Let’s get into it!
We know that depression risk increases during perimenopause, and epidemiologist have documented a 1.5-3 fold greater risk of first onset of depression and recurrent depression in women in perimenopause compared to those who are premenopausal or postmenopausal. I tell women this means there is light at the end of the tunnel, things will potentially get better, but until then let’s acknowledge this statistic for perimenopause. Can peri/menopausal hormone therapy help? Potentially – observational studies have reported depressive symptoms after the discontinuation of peri/menopausal hormone therapy in about 5-10% of women.
There are a few mechanisms why this estrogen decline leads to issues with mood.
1. Estrogen modulates neurotransmitter synthesis and metabolism, the stress axis activation, neuroplasticity, epigenesis and immune system activation – all of these systems play a role in the development of depression.
2. Estrogen signaling through the estrogen receptor beta reverses depressive and anxiety like behaviors in animal models.
3. Estrogen helps modulate reward responsiveness. In depression, reward responsiveness is disturbed.
4. Declining estrogen levels are accompanied by decreases in medial frontal and temporo-occiptal metabolism. This could play a roll in affect dysregulation (in simpler terms – depressed people tend to have a “flat” or “blunted” affect).
Menopausal hormone therapy does not have an FDA indication to be used to treat depression, anxiety, or mood disorders. However, in our practice we see that it greatly improves mood. We know that estrogen decline in the brain leads to hot flashes or vasomotor symptoms or night sweats – whatever you want to call it it’s all the same process. This is occurring in the hypothalamys on KnDy neurons (pronounced “candy” how sweet). Night sweats interrupt sleep. Poor sleep negatively impacts mood. Negatively impacted mood can effect sleep. People with anxiety and depression actually have higher rates of bothersome hot flashes.
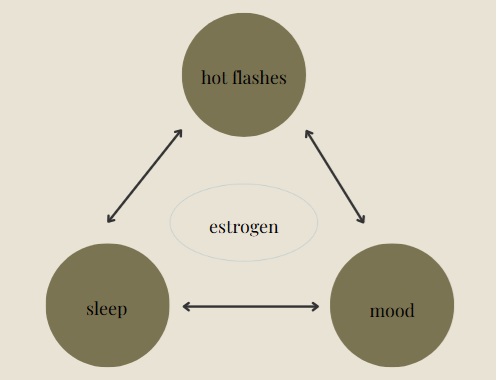
These 3 areas of symptomatology which all reside on the brain influence each other and are influenced by estrogen! So even if the jury is still out if estrogen therapy improves me (ie – no FDA indication for this yet), if we improve hot flashes and insomnia, mood will subsequently be impacted! In fact, a lot of times if we can fix the sleep issue, our patients report they just overall feel better.
And that’s what it’s all about!
Resources
Schmidt PJ, Ben Dor R, Martinez PE, Guerrieri GM, Harsh VL, Thompson K, Koziol DE, Nieman LK, Rubinow DR. Effects of Estradiol Withdrawal on Mood in Women With Past Perimenopausal Depression: A Randomized Clinical Trial. JAMA Psychiatry. 2015 Jul;72(7):714-26. doi: 10.1001/jamapsychiatry.2015.0111. PMID: 26018333; PMCID: PMC6391160.
https://womensmentalhealth.org/posts/new-research-study-at-the-cwmh-a-novel-treatment-for-menopausal-depression/
https://womensmentalhealth.org/posts/perimenopausal-depression/





